Abstract
Objective:
Brachytherapy employing iodine-125 seeds is an established treatment for low-risk prostate cancers. Post-implant dosimetry (PID) is an important tool for identifying suboptimal implants. The aim of this work was to improve suboptimal implants by a subsequent iodine-125 seed top-up (reimplantation), based on the PID results.
Methods:
Of 255 patients treated between 2009 and 2012, 6 were identified as having received suboptimal implants and were scheduled for seed top-up. Needle configurations and the number of top-up seeds were determined based on post-implant CT images as well as a reimplantation treatment plan. An average of 14 seeds per patient were implanted during each top-up. Dosimetric outcome was assessed via target parameters and doses received by organs at risk.
Results:
All six patients had a successful top-up, with a 67% increase in the mean dose delivered to 90% of the prostate volume and a 40% increase in the volume that receives 100% of the prescribed dose. However, the final dosimetric assessment was based on the same seed activity, as the planning system does not account for the decay of the initially implanted seeds. Although physical dosimetry is not influenced by different seed activities (doses are calculated to infinity), the radiobiological implications might be slightly different from the situation when optimal implantation is achieved with one treatment only.
Conclusion:
Seed reimplantation in suboptimal prostate implants is feasible and leads to successful clinical outcomes.
Advances in knowledge:
Suboptimal prostate implants can occur for various reasons. This work shows that seed reimplantation as salvage therapy can lead to an optimal dosimetric outcome with manageable normal tissue effects.
Low dose rate (LDR) brachytherapy employing radioactive seeds is a well-established treatment for low-risk prostate cancers. In our centre, implants are conducted with iodine-125 seeds (Oncura RAPID Strand, model 6711; Oncura Inc., Arlington Heights, IL) with an average seed activity of 0.395 mCi to deliver a prescribed dose of 145 Gy (to >98% of the prostate). Treatment planning and post-implant dosimetry (PID) are completed using SPOT-PRO™ v. 3.1 (Nucletron, Utrecht, Netherlands) software based on transrectal ultrasound images (for treatment planning) and CT images (for PID).
The most commonly reported parameters that are indicative of the dosimetric quality of the implant are D90 (the dose delivered to 90% of the prostate volume) and V100 (the volume that receives 100% of the prescribed dose). Several studies showed a link between the quality of implants and the biochemical outcome [1–3]. Therefore, to minimise the risk of recurrence, it is recommended to achieve a post-implant D90>140 Gy and V100>90% [1].
PID is an important quantitative tool for the assessment of LDR implants; therefore, it is recommended as a routine procedure by several professional organisations [2–5]. Besides evaluating the overall quality of the implant, PID can assist in the dosimetric assessment of the organs at risk (OARs). Although the dosimetry of OARs cannot be adjusted if overdosed, the radiation oncologist can have a closer follow-up of those patients at risk of developing normal tissue sequelae.
Another role of PID is to identify suboptimal implants that can arise owing to organ movement during the procedure, geographical misses of seeds or technical equipment errors. Despite all the efforts and experience of the brachytherapy team, suboptimal implants do occur and they have to be dealt with. Although several centres encounter such events, there is a lack of guidelines or even indications as to how to proceed to improve the final outcome. The major challenge is perhaps the planning, which cannot be done in a conventional way, i.e. based on the ultrasound study of the transrectal volume, owing to lack of previously implanted seed visibility [6]. Therefore, post-implant CT images are the most convenient to use for this task, as the original seeds can be seen and extra seeds can be added to cover the underdosed areas of the prostate.
The aim of this work was to present our experience with iodine-125 seed reimplantation (top-up) in a cohort of six patients whose initial implant was suboptimal as identified by PID. The technical and dosimetric challenges of seed top-up implants are investigated.
MATERIALS AND METHODS
Of 255 patients treated with iodine-125 permanent seed brachytherapy between January 2009 and July 2012 at the Royal Adelaide Hospital, SA, 6 were identified as having received suboptimal implants and were scheduled for seed top-up. The suboptimal implants were attributed to equipment/technical problems (two cases), patient movement during implantation (one case) and uncommonly large oedema (one case); however, for two patients, the causes of underdosage were unidentified. Therefore, the cold spots were random from patient to patient, although underdosage of the base was more common than the involvement of other prostate regions.
The decision to undergo reimplantation was based on the PID results using ultrasound–CT image coregistration, which our centre’s standard technique (the methods are described in detail in a previous report [7]). However, in all situations, the main dosimetric parameters were independently confirmed by a second medical physicist, and in some cases, when the result was uncertain, an alternative PID technique was also used, such as CT-delineation-based PID or MR–CT image coregistration-based PID. As with all our PID data, the results were reviewed by the patient’s radiation oncologist, who, after following the PID prostate D90 criteria given below, decided whether the patient should be scheduled for a seed top-up or not.
At our centre, we categorise the quality of the implants according to the following PID D90 values:
D90>145 Gy—good implant [as recommended by Groupe Européen de Curiethérapie–European Society for Radiotherapy & Oncology (GEC-ESTRO) guidelines] [5]
130 Gy<D90<145 Gy—adequate by local definition (within 10% of the prescribed dose).
110 Gy<D90<130 Gy—potentially acceptable, subject to re-assessment of PID with another PID technique and evaluation of cold spots. If cold spots are identified in areas that were not positive on transrectal ultrasound biopsy, we consider the implant acceptable. If the implant is subsequently deemed inadequate, the patient is scheduled for a seed top-up procedure.
D90<110 Gy—the implant is inadequate [1,5]. The patient is scheduled for a seed top-up procedure.
For those patients identified as having an inadequate implant, a top-up treatment plan is generated. This is designed using the initial PID ultrasound–CT images as the reference to determine the location and the number of seeds required to improve the dosimetry.
The prostate target (hereafter referred to as the target) is defined as the clinical target volume, and acceptable target volumes for initial implants are between 15 and 55 cm3. A planning target volume (PTV) is also defined during preplanning but is not considered in this report, as its dosimetry trends reflect those of the target values.
Method of setting up the seed top-up plan
This is perhaps the most demanding step in the reimplantation process owing to the limitations of the treatment planning system (as will be discussed later). Some explanations of our PID technique are first required to help understand the seed top-up planning method.
The PID CT images are scanned at 2-mm slice thickness and 2-mm spacing. As described in the study by Marcu et al [7], the PID CT images are coregistered (matched) to the pre-implant ultrasound images, with the image fusion module of the SPOT-PRO treatment planning system, by manually shifting and rotating the overlaid image sets until anatomical references are aligned. Once image sets are matched, the target and PTV from the ultrasound images are copied onto the CT images; the rectum and urethra are drawn directly onto the CT images. Subsequent analysis of the PID is performed on the CT images with the copied and drawn contours. Following computerised seed identification, the PID is assessed.
Analysis of the PID dose–volume histogram (DVH) data and visual dose coverage identifies the “cold spots” (areas of target receiving less than the prescription dose) and potential areas that require a top-up of seeds. The two main problems that arise with relating the planned positioning of the top-up seeds to the actual desired positions for implant are: (1) the orientation of the CT images and (2) the implant template grid pattern.
(1) Orientation of the CT images: as the CT is performed with the patient supine and the ultrasound is performed with the patient in the lithotomy position, the orientation of the prostate and local anatomy is different in each setting. Although this can be overcome for the purposes of matching two data sets together for copying contours, it presents a problem for determining the seed/needle locations when viewing the CT data set in the planning module. If we assume that the ultrasound data set is the normal orientation, then the CT data set is rotated (approximately 20–40°) about the patient's left/right axis during the matching process; however, when subsequently viewing the CT images in the post-implant planning module, the CT images are in their normal scanned orientation. This means that the needle tracks are not in the horizontal plane, when viewed laterally, but angled anteriorly in the inferior to superior direction (Figure 1). This therefore causes problems with relating possible top-up seed locations (as determined from the CT images) to their equivalent positions when viewed on the ultrasound.
Right lateral views of post-implant CT images at various positions through the prostate. The superimposed manually added lines indicate the needle tracks for the visible seeds. Also visible are the target and planning target volume contours. The central image shows the catheter balloon with contrast and a part of the urethra contour.
The following paragraph describes the method implemented in our department using the SPOT-PRO software. Nevertheless, the essentials of the process could be easily adapted for use with other brachytherapy treatment planning systems. Firstly, we scroll through the lateral CT images and determine the angle of the implanted needles by visualising the seed positions. As the seeds are implanted in the Rapid Strand form, we have confidence in identifying their corresponding needle tracks. Figure 1 shows some superimposed lines that help to illustrate this. Once the angle is determined, we then adjust the CT data set such that we can visualise the transverse CT images that are perpendicular to the angle of the needle tracks.
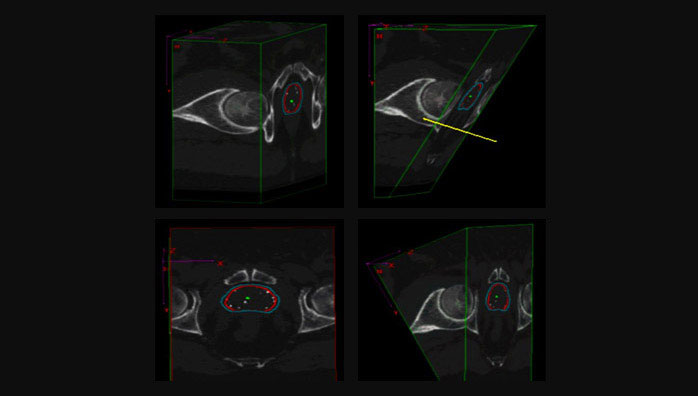
To achieve this, we use the three-dimensional cube facility within the SPOT-PRO software. Figure 2 demonstrates the steps involved in changing the transverse views from the original to those that are perpendicular to the angle of the needle tracks. The CT needle tracks would now be horizontal if viewed laterally. When we now scroll through the angle-corrected transverse views, they are in the same orientation as the transverse views in the original treatment plan of the ultrasound images. Therefore, determining grid positions for the top-up seeds/needles is achievable.
Demonstration of the steps involved in changing transverse CT images from the normal axial orientation to that which is perpendicular to the needle tracks. Starting from top left in clockwise rotation: a transverse image through the prostate is established within the three-dimensional (3D) cube image set, next a cut plane is created through the image set at an angle perpendicular to the angle of the needle tracks (as shown in Figure 1 and indicated by the protruding line), then the 3D cube is rotated so that the angle-corrected transverse slice is vertical; this is followed by a further rotation to visualise the angle-corrected transverse slice in the conventional way.
(2) Implant template grid pattern: unfortunately, the treatment planning system does not show the implant template grid pattern on the CT images, so mapping out the needle locations according to this grid can be difficult. However, after following the steps above to orientate the post-implant CT images, the grid positions can be determined by simultaneously viewing the CT images and the ultrasound images by using the target contour and seeds as the common reference guide. In the case of the SPOT-PRO planning system, this cannot be done on screen, so we print out a selection of transverse ultrasound images with the template visible and scroll through the CT images on screen. In addition, the base and apex of the target can be identified and compared, so that the depth of needle insertion (for seed deployment) can be determined.
The top-up seeds are then added to the plan (with known potential grid positions) until the cold spots are sufficiently covered with target and satisfactory OAR DVH values. The patients are notified of the treatment outcome and advised that they should undergo a reimplantation procedure. The procedure is guided by transrectal ultrasound and seed deployment is checked on fluoroscopic images, where the previously implanted seeds are also visible. Fluoroscopic guidance is particularly useful in those situations where the underdosage occurs in the base of the prostate, and the new baseline enables a good dosimetric coverage of that area. Dosimetric outcome of the top-up implant is assessed, the following day, via a second post-implant CT scan, coregistered to the original pre-implant ultrasound images as done previously with the initial PID CT. Target parameters (D90 and V100) and doses received by OAR, i.e. urethra [the dose delivered to 10% of the prostatic urethra (D10) and the dose delivered to 30% of the prostatic urethra (D30)] and rectum [the dose to 0.1 cm3 of the rectum (D0.1 cm3) and the dose to 2 cm3 of the rectum (D2 cm3)], are assessed and are reported later.
RESULTS
Number of seeds implanted and the time interval between implants
The number of seeds needed for the initial implant as well as the extra number of seeds used for top-up for all six patients is listed in Table 1. An average of 14 seeds per patient was implanted during each top-up. Table 1 also lists the time interval between the implant and the top-up day. Depending on the waiting list and also the patient’s availability, the top-up was scheduled, on average, within 3 months after the implant.
Table 1.
Seed top-up data
| Patient number | Target volume (cm3) | Number of seeds originally implanted | Number of seeds implanted during top-up | Time interval between the implants (days) |
| 1 | 28 | 67 | 8 | 21 |
| 2 | 26 | 73 | 12 | 49 |
| 3 | 37 | 85 | 18 | 141 |
| 4 | 33 | 76 | 11 | 85 |
| 5 | 42 | 61 | 18 | 91 |
| 6 | 30 | 59 | 18 | 63 |
| Average | 32 | 70 | 14 | 75 |
Target dosimetry before and after the top-up
Individual charts showing the target implant dosimetry and the dosimetry after the top-up are represented in Figures 3 and and4.4. The improvement in dosimetry is clearly observed.
Dose delivered to 90% of the prostate volume (D90) target values before and after the top-up individually shown for the six treated patients.
Volume receiving 100% of the prescribed dose (V100) target values before and after the top-up individually shown for the six treated patients.
Figures 3 and and44 illustrate that, if the cold spots had been covered from the initial implant, the main dosimetric parameters D90 and V100 would have significantly increased. Therefore, although the dose to target after the top-up leads to an average D90 of 150 Gy (which represents a 67% increase when compared with the implant dosimetry), the volume to be covered by 100% of the prescribed dose (V100) increased by 40%, reaching an average of 92% for the six studied patients.
All patients but one had D90>140 Gy and V100>90%. Patient 3 had an initial D90=43.5 Gy, increasing to D90=124 Gy after reimplantation. Although the dosimetry is still below the recommended limit, the diseased areas, as proven by biopsies, were all well implanted and the corresponding cold spots were adequately covered. Since the urethral dose was already high before the reimplantation (D10=203 Gy and D30=185 Gy), after the addition of top-up seeds the urethral dose exceeded the recommended safety limits (D10=243 Gy and D30=221 Gy). Thus, to avoid increasing the risk for toxicities, the plan had to be compromised.
Organs-at-risk dosimetry before and after the top-up
The dosimetric evaluation of the OARs was undertaken using the GEC-ESTRO recommendations whereby the urethral primary dosimetric parameter, D10, should be <150% of the prescribed dose and the secondary parameter, D30, should be <130% of the prescribed dose [5].
Urethra
The urethral dose related to D10 reached values above the recommended limit for two patients, while according to the secondary dosimetric parameter, D30, three patients received higher doses than recommended limits, as a compromise for a better tumour dosimetry (Table 2).
Table 2.
Post-top-up dosimetry for target and organs at risk
| Patient number | Target (prostate) | Prostatic urethra | Rectum | |||
| D90 (Gy) | V100 (%) | D10 (Gy) | D30 (Gy) | D0.1 cm3 (Gy) | D2 cm3 (Gy) | |
| 1 | 156.7 | 93.3 | 176.4 | 164.6 | 232.8 | 124.3 |
| 2 | 142.4 | 89.4 | 204.5 | 183.6 | 189.2 | 112.9 |
| 3 | 124.0 | 85.5 | 243.0 | 221.0 | 236.0 | 94.0 |
| 4 | 168.3 | 95.6 | 274.2 | 228.6 | 205.0 | 120.0 |
| 5 | 148.5 | 91.6 | 219.4 | 202.1 | 296.0 | 169.0 |
| 6 | 159.0 | 94.0 | 199.0 | 187.0 | 155.0 | 68.0 |
| Mean value (standard deviation) | 150 (±15) | 92 (±4) | 219 (±35) | 198 (±24) | 219 (±48) | 115 (±34) |
| Recommended limits | >145 | >90% | <218 | <189 | <200 | <145 |
D10, dose delivered to 10% of the prostatic urethra; D30, dose delivered to 30% of the prostatic urethra; D90, dose delivered to 90% of the prostatic urethra; D0.1 cm3, dose to 0.1 cm3 of the rectum; D2 cm3, dose delivered to 2 cm3 of the rectum; V100, volume receiving 100% of the prescribed dose.
Rectum
Similarly to the prostatic urethra, the dosimetric requirements for the rectum were established based on the GEC-ESTRO recommendations [5]. Therefore, D2 cm3<145 Gy was used as a primary parameter and D0.1 cm3<200 Gy was used as a secondary parameter. One patient had D2 cm3=169 Gy after top-up, whereas, for all the others, the primary dosimetric parameter for the rectum was kept below the 145-Gy limit (Table 2). When assessing the secondary dosimetric indicator, it was noticed that four out of six patients received D0.1 cm3 above the recommended 200 Gy (Table 2). However, two of these patients already had elevated levels before the top-up owing to geographic misplacements of seeds during the original implantation. These patients underwent a closer follow-up to ensure minimum discomfort owing to possible treatment-related side effects. However, no rectal morbidities have been reported so far.
Summary of dosimetry data before and after the top-up
All six patients had a successful top-up, with a 67% increase in the mean D90 value and a 40% increase in V100. Unavoidably, doses to OARs have increased as well, in some cases exceeding the recommended limits. It should be noted that the final dosimetric assessment (implant+top-up) was based on the same seed activity (0.395 mCi), as the planning system does not account for the decay of the initially implanted seeds. The DVH values obtained post top-up are presented in Table 2 both for the target and for the OARs. Table 2 also shows the recommended limits for these structures. It should be noted that, through the top-up procedure, the dose to the target was increased to enable good tumour control, while as a compromise, for the OARs, some values were marginally higher than the recommended limits.
DISCUSSION
There are two main challenges involving the top-up procedure and its outcome: one covers the physical aspect of seed dosimetry and the other relates to the radiobiological implications of the top-up.
- (1)
Some planning systems, such as the one used in the current study, do not allow treatment plans with different seed activities related to different implant dates. This means that although on the implant day the average seed activity was 0.395 mCi, by the time of the top-up implant these seeds have decayed by an amount which depends on the time gap between the implant and the top-up day. However, the top-up was conducted using 0.395 mCi seeds, as for the implant; thus, for dose calculation SPOT-PRO assumes that all seeds were implanted on the same date and with the same activity. Despite this discrepancy between the two implanted seed batches used in the dose calculation, any potential differences in physical effect owing to the dose delivered is probably not important for iodine-125 seeds of the same strength but implanted at different times (provided that top-up is given within a couple of isotope half-lives), as they would yield the same cumulative (physical) dose after 2 years (knowing that 80% of the total dose is delivered in about 140 days), to within <0.1%. In our case, the SPOT-PRO dose calculation algorithm uses 10 half-lives to determine the cumulative dose, so any discrepancy in the dose displayed on the plan relating to the different seed activities or dates is insignificant (again provided the top-up is given within 2 isotope half-lives).
- (2)
Radiobiological effects could be influenced by the time difference between the two implant dates as the 145-Gy prescribed dose is delivered in two separate sessions, thus over a longer time period than initially planned (Figure 5, in which the dose rate over time is calculated considering that the initial dose rate for iodine-125 is about 7 cGy h–1 [8]). Although patient 1 had his top-up 21 days after implant, thus well within the half-life of iodine-125, and when the dose rate was 5.5 cGy h–1, patient 3 underwent the seed boost 141 days after the implant (owing to logistics problems), at a time when the initially implanted seeds decayed with a dose rate of 1.35 cGy h–1, delivering the remaining 20% of the prescribed dose.
Nevertheless, considering that permanent seed implants are conducted on patients with low-risk and low-grade prostate cancer, the time gap between the implant and the top-up might not induce any radiobiological events that differ from a single procedure.
Our study was based on the dosimetric evaluation of post-implant CT images registered to ultrasound images. Although this image coregistration was the most convenient in our situation, we acknowledge the fact that fused post-implant CT/MR images registered to ultrasound images are most likely to be the optimum [8,9].
There are limited studies in the literature recommending an external beam radiotherapy (EBRT) boost for suboptimal implants. One such study suggests salvage EBRT using a multimodality dose summation between intensity-modulated radiotherapy and brachytherapy dose matrices by overcoming the challenges imposed by planning systems [10]. For this task, Bice et al [11] have used image coregistration employing a post-implant CT and ultrasound volume study. In their study, the dosimetric results of the original implant were overlaid on the salvage plan and the total doses to the target and the OARs were evaluated. The main dosimetric parameter reported was V80, which improved from an average of 56% to 93%.
We suggest that LDR seed reimplantation for suboptimal implants presents certain advantages over an EBRT boost. Therefore, when compared with an EBRT boost, LDR top-up offers a better dosimetric outcome owing to more accurate targeting of the cold spots. In addition, the dosimetry and radiobiology of a composite LDR brachytherapy/EBRT plan still remains a challenge for many treatment planning systems. Regarding the dose to OARs, with LDR top-up, the added urethral dose can be kept to a minimum with careful placement of seeds, as compared with EBRT when the urethra would almost certainly be included in the radiation field. Also, an advantage from the patient’s perspective is that only one visit is required for treatment, instead of several visits, which a fractionated EBRT would require.
A salvage reimplantation technique for suboptimal implants was reported by Hughes et al [6] using fluoroscopic guidance, whereby an underdosed base owing to systematic seed misplacement led to a V100=46%. For better localisation of the seeds to be implanted, a grid was superimposed on the original post-implant CT images and digitised into the planning system to facilitate dosimetric evaluation (similar to planning on transrectal ultrasound images). The reimplantation results showed V100=98%, although with increased urinary morbidity.
Keyes et al [12] have described the salvage implants undertaken on seven patients with poor initial dosimetry. Their planning simulation principle was similar to the one reported in the current work, whereby extra seeds were simulated on the underdosed areas of prostate on post-implant CT images, maintaining the original 5-mm distance between seeds. A composite dose was determined by adding the doses for the two implants together, without taking into account the radioactive decay of the initially implanted seeds.
A recent case report has described the salvage reimplantation of a suboptimally implanted prostate cancer patient by employing post-implant CT guidance and real-time intra-operative planning using loose seeds [13]. PID revealed an underdosed base, leading to D90=92.9 Gy and V100=71%, which after the addition of 20 seeds increased to D90=173.24 Gy and V100=96.88%. The flexibility of intra-operative planning has allowed continuous adjustments of seed positioning, thus making this technique suitable for salvage implants.
As a drawback, LDR top-up is labour intensive and involves a large team of professionals to actively participate in treatment preparation and delivery. Furthermore, the patient requires a second general anaesthetic, which might be a problem for those patients with an underlying condition. Also, since patients might live in other cities, thus a long distance from the hospital, top-up sessions would have to accommodate their travel arrangements, which might sometimes delay the boost implant. Nevertheless, the same problem might be encountered if EBRT is chosen as boost treatment.
CONCLUSION
PID is a valuable tool in assessing the quality of an implant. Despite all team efforts taken to achieve high-quality implants, every so often implants can be suboptimal owing to technical-, staff experience- or patient-related matters.
To correct the dosimetry of an unsatisfactory implant, a top-up procedure was implemented in our centre, involving the implantation of extra seeds to account for the cold spots and other geographical misses. A description of the methods used to overcome the technical difficulties in planning top-up implants has been presented.
Although the final target dosimetry achieved was satisfactory, the procedure was compromised by higher doses being delivered to the OARs than the recommended limits. The affected patients are kept under close observation to identify and treat any normal tissue toxicities.
In conclusion, we found that iodine-125 seed top-up is a feasible method for improving the quality of a previous suboptimal implant.
ACKNOWLEDGMENTS
The authors would like to acknowledge the radiation oncologists, urologists, radiation therapists, medical physicists, nursing staff and all other members of the prostate brachytherapy team at the Royal Adelaide Hospital for their dedication to the prostate brachytherapy service over the years.
The information comes from:
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3664978/